Hepatitis C and Iron
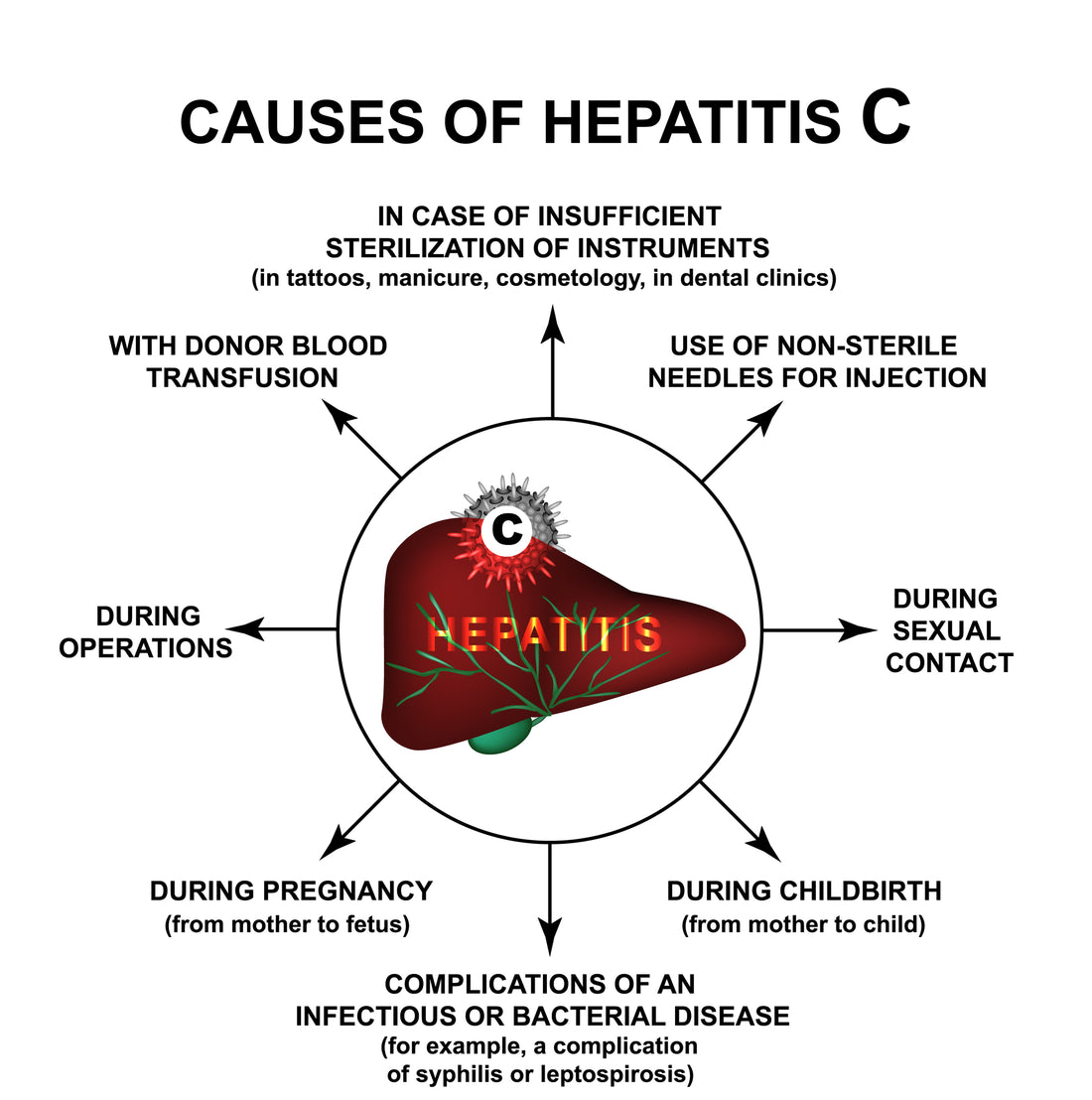
Over 4 million Americans have been infected with the hepatitis C virus (HCV). Hep C infects the liver and is responsible for 10,000 - 12,000 deaths each year.
The liver is the critical organ in the body for the metabolism of iron. Excess iron in the body can be very damaging.
Patients with chronic hepatitis C often have an increase of iron concentration in the liver. Iron load may have a serious effect on HCV infection, and in turn, the HCV may alter regulation of iron homeostasis.
Iron Overload and Hepatitis C
One of the critical factors in HCV progression is iron overload, which is commonly seen in people suffering from chronic Hepatitis C. Increased iron levels in the liver may contribute to the severity of the disease, affect treatment responses, and increase the likelihood of developing liver cancer. Here's a deeper look at the facts:
How Iron Affects the Liver in Hepatitis C Patients
The liver plays a vital role in iron metabolism, and excess iron can damage liver cells. Many patients with chronic Hepatitis C have higher levels of iron in their liver, which can exacerbate the disease. The iron load in the liver may speed up HCV progression and even interfere with immune responses that are necessary to control the infection.
Iron Overload and Risk of Advanced HCV Disease
The Role of Oxidative Stress and Cellular Immunity
Iron overload is not only an issue of excess iron in the liver but also how that iron causes oxidative stress, which can damage liver cells. In people with Hepatitis C, high iron levels increase oxidative stress, which worsens inflammation and may promote the virus's growth. This, in turn, increases the risk of liver damage and liver cancer.
Moreover, the excess iron impairs cellular immunity, reducing the body’s ability to fight off the virus. It’s essential for Hepatitis C patients to manage their iron levels to reduce these harmful effects.
Impact on Treatment Response: Iron Levels and Interferon Therapy
Studies have shown that patients with higher iron levels may have a reduced response to interferon therapy, which is one of the standard treatments for Hepatitis C. Patients with high iron levels tend to respond poorly to treatment, making it harder to clear the virus from their system.
Line Graph: Treatment Response Rate vs. Iron Levels
Many studies about the relationship between iron and HCV are inconclusive because there are so many factors to rule out — such as race, gender, age and stage of the disease, and the genetic mutation of the HFE gene present in hemochromatosia — all of which profoundly affect results.
It is also challenging to determine whether the increased iron levels seen in individuals with cirrhotic HCV facilitate progression toward end-stage liver disease or are a result of increased iron in the cirrhotic liver.
But almost all studies suggest that iron overload is associated with more advanced HCV disease, poor response to interferon monotherapy, and increased risk of liver cancer. In some studies, increased iron has actually been shown to enhance the growth of the hepatitis C virus in the laboratory. There is also general agreement about the likelihood that iron overload worsens liver disease in HCV through oxidative stress and affecting cellular immunity. It has also been found that it is not just the amount of iron in the liver that is important, but also the distribution of the iron within an HCV-infected liver.
Liverdisease.com, suggests, that people with chronic HCV whose serum iron level is elevated, or who have cirrhosis, should probably avoid taking iron supplements. In addition, it suggests they should restrict their intake of iron-rich foods, such as red meats, liver, and iron-fortified cereals, and should avoid cooking with iron-coated cookware and utensils. Iron depletion therapy may be indicated to delay disease progression.
Lifestyle and Dietary Changes for Hepatitis C Patients
According to research, iron restriction is one of the most effective ways for HCV patients to manage iron overload. This includes avoiding iron supplements, cutting back on iron-rich foods like red meats and liver, and even avoiding cooking with iron-coated cookware.
Iron Depletion Therapy may also be considered for some patients to delay the progression of liver disease. This therapy involves reducing iron levels through methods like phlebotomy, which removes iron from the body.
Key Takeaways
- Iron overload is associated with advanced HCV disease, a poor response to therapy, and an increased risk of liver cancer.
- Managing iron levels is essential for reducing liver damage and improving treatment outcomes.
- Patients should work with their healthcare provider to monitor iron levels and make appropriate lifestyle changes, including dietary adjustments and possibly iron depletion therapy.
As new studies continue to emerge, we’ll likely see more developments on how to best manage iron overload in HCV patients.
Conclusion
By managing iron levels and adopting a healthy lifestyle, Hepatitis C patients can reduce the risk of liver damage and improve treatment outcomes. The complex relationship between iron and Hepatitis C highlights the importance of ongoing research and individualized care.
Stay tuned for updates on the latest studies and recommendations for managing iron levels in Hepatitis C.
As scientific and medical studies continue to explore the relationship between iron and HCV, new recommendations are likely to surface.












